|
2/19/2023 0 Comments Gram positive cocci in clusters However, antimicrobial use may predispose patients to acquiring MRSA colonization or infection if they are exposed to the organism. Second, the fact that there are relatively few clones of MRSA worldwide suggests that person-to-person spread, not antimicrobial use, is the most important factor in the spread of MRSA. In addition, colonized or infected healthcare workers (HCWs) and contaminated items in the environment can also serve as reservoirs for MRSA. Given this background information, what are the key concepts regarding prevention and control of MRSA transmission and infection? First, the reservoir for MRSA is primarily colonized or infected patients. Prevention and control of methicillin resistant Staphylococcus aureus aureus, thereby rendering the vancomycin inactive. aureus cell walls trap vancomycin before it reaches the cytoplasmic membrane of S. Some investigators have hypothesized that thick S. The molecular mechanism of intermediate vancomycin resistance is not fully understood. aureus isolate that has one subpopulation that is vancomycin susceptible according to current CLSI breakpoints and a subpopulation that grows in the presence of vancomycin. aureus isolate with a vancomycin minimum inhibitory concentration greater than the Clinical and Laboratory Standards Institute (CLSI) break point of 4 μg/ml and hVISA is defined as a S. VRSA is defined as an MRSA isolate that carries the VanA gene. aureus (VRSA) have emerged around the world. aureus (VISA) and heterogeneous VISA (hVISA), and the fully resistant vancomycin-resistant S. Since 1997, both vancomycin-intermediate S. aureus have made vancomycin a less appealing option. However, rare cases of vancomycin resistance among S. Risk factors for acquisition of MRSA include: comorbidities such as HIV and renal failure, dialysis, severe illness, intensive care unit (ICU) admission, previous admission to a hospital, injection drug use, and residence in a long-term-care facility, incarceration, living in crowded conditions, and poor hygiene.Ĭurrently, vancomycin is the most frequently prescribed antimicrobial therapy for MRSA bacteremia. Several hypotheses may explain this association: MRSA bacteremia is associated with higher mortality rates than is methicillin-susceptible S. aureus clinical isolates in US hospitals are methicillin resistant. Thus colonization, while increasing infection risk, may actually protect patients who become infected from dying. This finding was possibly due to up-regulated immune responses in colonized patients or to lower virulence of colonizing strains compared with infecting strains. However, a study by Wertheim et al., demonstrated that all cause and bacteremia-related deaths were significantly higher among patients who were not colonized compared with those who were colonized before their bacteremias, even though colonization was a strong risk-factor for bacteremia. aureus infections, compared with patients who were not colonized. aureus were more likely to acquire healthcare-associated (HA) S. 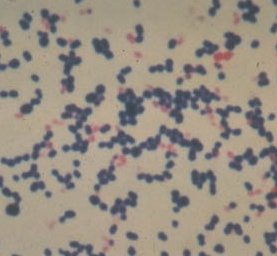
Enterococcus (e.g.Previous studies have found that patients colonized with S.Staphylococus lugdunensis should raise concerns for endocarditis with a single positive blood culture Ĭhains or Pairs ( Strep Species and Related).Rare cause of endocarditis, meningitis, and Skin and Soft Tissue Infections.Most common skin contaminant found in blood cultures.Most common cause of catheter-related bacteremia.Always consider as true bacteremia (and not a contaminant) due to the danger of delaying treatment.“Branching Gram positive rods, modified acid fast stain positive” may suggest Nocardia or Streptomyces species."Gram positive cocci in pairs and chains" may suggest Streptococcus species or Enterococcus species.“Gram positive cocci in clusters” may suggest Staphylococcus species.2.2 Chains or Pairs (Strep Species and Related). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
